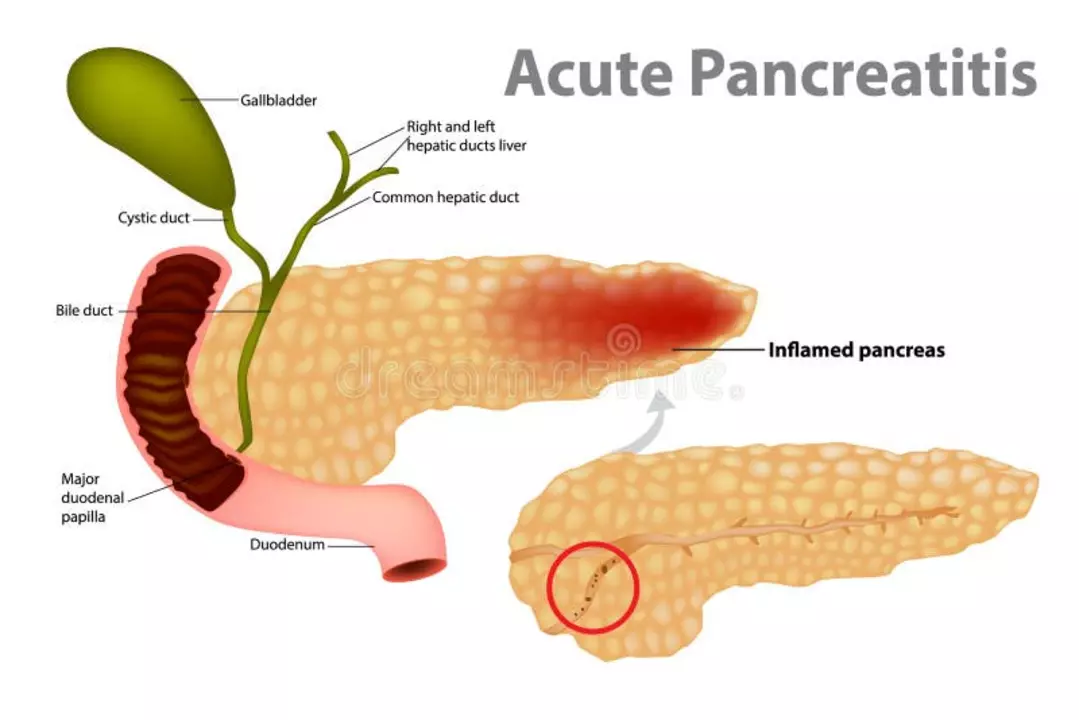
Pancreatitis: What to watch for and how to act
Pancreatitis means inflammation of the pancreas. It can show up suddenly (acute) or slowly over time (chronic). Both can hurt your digestion, cause belly pain, and lead to serious complications if you ignore warning signs. Here’s a simple, practical guide to recognize pancreatitis and take smart next steps.
Common causes and how they matter
Two causes account for most cases: gallstones and heavy alcohol use. Gallstones can block the bile duct and trigger inflammation. Drinking too much for a long time can damage the pancreas. Other causes include very high triglycerides, some medications, infections, trauma, and certain medical procedures. If you have risk factors (gallstones, high triglycerides, recent heavy drinking), mention them right away to your doctor—it changes testing and treatment.
What pancreatitis usually feels like
The most common symptom is steady, intense pain in the upper belly that often radiates to the back. The pain can get worse after eating, especially fatty meals. Nausea, vomiting, fever, rapid heartbeat, and a swollen belly are common too. Chronic pancreatitis may cause ongoing discomfort, weight loss, and greasy stools caused by poor fat absorption.
If you have sudden, severe belly pain with vomiting, lightheadedness, or trouble breathing, get urgent care. Those can be signs of a severe attack that needs immediate treatment.
Doctors use blood tests (amylase and lipase) and imaging (abdominal ultrasound or CT scan) to confirm pancreatitis and look for causes like gallstones. Sometimes an endoscopic test (ERCP) is needed to remove a blocked stone.
Simple steps for recovery and prevention
Initial hospital care often includes fasting (to rest the pancreas), IV fluids, and pain control. Most people improve after 48–72 hours with this basic care. After the acute phase, focus on practical things you can control:
- Avoid alcohol completely. Even small amounts can trigger another attack.
- Eat a low-fat diet and spread meals into smaller portions if your doctor recommends it.
- Control high triglycerides with diet, exercise, and medications if needed.
- Quit smoking—smoking speeds up chronic damage.
- Follow up with a gastroenterologist for tests, pancreatic enzyme support, or diabetes checks if the pancreas is damaged.
Chronic pancreatitis can require enzyme replacement to help digest food and extra calories to prevent weight loss. Your doctor can advise on supplements and pain options that are safe for long-term use.
Knowing the signs and acting fast saves time and prevents complications. If you suspect pancreatitis, tell your doctor about alcohol use, gallstone history, and recent medications. That makes diagnosis quicker and treatment safer.
Want more articles about medications, tests, or how to find safe online pharmacies for prescriptions related to pancreas care? Explore our guides and tools to make informed choices about treatment and follow-up.
Gallstones and Pancreatitis: Understanding the Connection
In my recent research on gallstones and pancreatitis, I discovered a fascinating connection between the two conditions. Gallstones, which are hard deposits in the gallbladder, can sometimes block the ducts that release digestive enzymes from the pancreas, leading to pancreatitis. This inflammation of the pancreas can be extremely painful and even life-threatening in severe cases. It is essential to be aware of the symptoms, such as abdominal pain, fever, and nausea, and seek medical help if you suspect gallstones or pancreatitis. By understanding this connection, we can take steps to prevent and manage these conditions effectively.
VIEW MORE