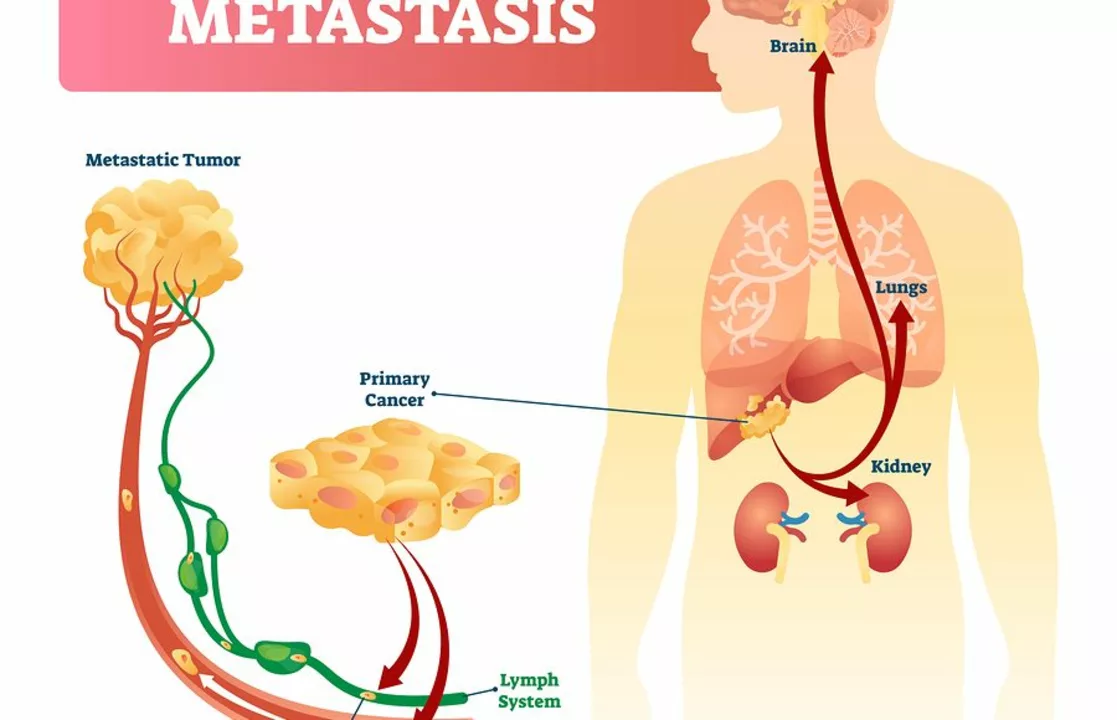
Metastatic cancer — what it means and what to do next
Hearing the word "metastatic" can feel overwhelming. Metastatic cancer simply means cancer cells from the original tumor have moved to other parts of the body. That usually puts the disease at stage IV, but stage IV doesn’t mean there are no options. Many people live months or years with good symptom control and meaningful time with family. This page gives practical, no-nonsense steps to understand diagnosis, treatment choices, and daily life.
How metastatic cancer is diagnosed
Doctors use scans and tests to find where the cancer spread. Common tools are CT, MRI, PET scans and targeted biopsies. Blood tests, tumor markers, and genetic profiling of the tumor also guide treatment. If you’re collecting records, ask for copies of scan reports, pathology notes, and the exact results of any genetic tests—those details matter when choosing targeted drugs or enrolling in trials.
Treatment options you’ll hear about
Treatments for metastatic cancer aim to control growth, reduce symptoms, and maintain quality of life. Options include systemic therapies (chemotherapy, targeted therapy, immunotherapy, or hormonal therapy), local control (surgery or radiation to relieve pain or stop a single growing lesion), and supportive care to manage side effects. Which path is best depends on the tumor type, mutations found on testing, where it spread, and what you want from treatment.
Ask your doctor these straightforward questions: What is the goal of this treatment—shrink the tumor, slow spread, or ease symptoms? What are realistic benefits and most likely side effects? Are there targeted therapies or trials that match my tumor’s profile? Would a second opinion help? If possible, bring a family member to appointments to help remember answers.
Practical tips for patients and caregivers
Start a single folder (paper or digital) with contact info, scan dates, treatment summaries, and medication lists. Use the patient portal to download results. Track symptoms with a simple daily note—date, pain level, appetite, and medications taken. That log helps your team adjust doses and manage side effects faster.
Consider palliative care early; it’s not only for the last days. Palliative specialists focus on pain, breathlessness, fatigue, and mood—things that make life harder, not the cancer itself. Ask your oncologist to help set that up. Also look into clinicaltrials.gov or your cancer center’s trial list if you want access to new drugs.
Find support: local support groups, online communities for your cancer type, and social workers at the hospital who can help with finances and home care. Small, daily wins—better sleep, less nausea, a short walk—add up. Keep asking questions, keep records, and get help when you need it. You don’t have to manage this alone.
The role of capecitabine in the management of metastatic cancer
As a blogger, I've recently researched the role of capecitabine in the management of metastatic cancer. Capecitabine is an oral chemotherapy drug that has proven to be effective in treating various types of metastatic cancers, including breast and colorectal cancer. It works by inhibiting the synthesis of DNA in cancer cells, ultimately slowing down or stopping their growth. The convenience of taking capecitabine orally, as opposed to intravenous chemotherapy, has been a game-changer for cancer patients, allowing them to receive treatment in the comfort of their own homes. Overall, capecitabine has become a critical component in managing metastatic cancer and improving patients' quality of life.
VIEW MORE