Gallstones: what they feel like and what to do
Half of people with gallstones never know they have them. But when a stone blocks a bile duct, the pain can be brutal. This page gives clear, practical steps so you know when to worry, which tests to expect, and what actually helps prevent new stones.
Symptoms and when to get help
The classic sign is a sudden, intense pain in the upper right belly that can last 30 minutes to several hours. Pain often radiates to the back or right shoulder blade. Other warning signs: nausea, vomiting, fever, yellow skin or eyes (jaundice), dark urine, or light-colored stools. If you have high fever, persistent vomiting, or jaundice, get emergency care—those signs can mean infection or bile duct blockage.
Not every belly ache is a gallstone. Doctors look for a pattern: severe, crampy attacks after fatty meals or at night that come and go. If you’re unsure, a quick call to your clinic can help decide if you need urgent care or an appointment.
How doctors diagnose gallstones
Most teams start with an abdominal ultrasound. It’s fast, painless, and shows stones inside the gallbladder. Blood tests check for infection, liver or bile-duct problems. If ultrasound is unclear, your doctor might order a HIDA scan, CT, or MRCP to see the bile ducts and gallbladder in more detail.
Found a stone but no symptoms? Many people are fine with watchful waiting. Active treatment targets people with repeated attacks or complications like cholecystitis (inflamed gallbladder), pancreatitis, or cholangitis (infected bile ducts).
Surgical removal of the gallbladder (laparoscopic cholecystectomy) is the most common fix. It’s routine and most people recover quickly and eat normally afterward. If surgery isn’t an option, there are medicines like ursodeoxycholic acid that can dissolve some cholesterol stones, but treatment takes months and stones can come back. Shock-wave lithotripsy is rarely used and only fits select cases.
Preventing gallstones is practical: keep a healthy weight, but avoid crash diets—rapid weight loss raises your risk. Aim for steady loss (about 1–2 pounds per week). Eat regular meals with fiber-rich foods, healthy fats (olive oil, fatty fish), and limit refined carbs and large amounts of saturated fat. Some studies suggest moderate coffee intake may lower risk, but don’t start heavy drinking for that reason.
If you have risk factors—female, over 40, obesity, pregnancy, certain medications, or a family history—mention them to your doctor. Small changes to diet and weight loss pace can make a real difference. And if pain hits hard or you develop fever/jaundice, don’t wait: get medical care fast.
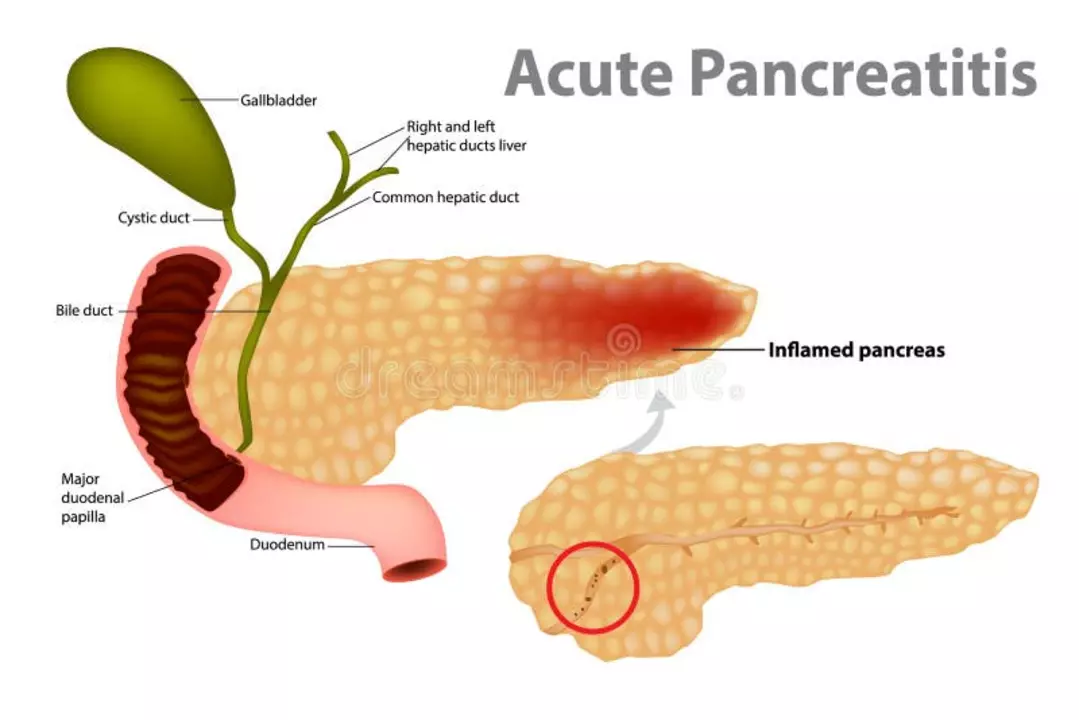
Gallstones and Pancreatitis: Understanding the Connection
In my recent research on gallstones and pancreatitis, I discovered a fascinating connection between the two conditions. Gallstones, which are hard deposits in the gallbladder, can sometimes block the ducts that release digestive enzymes from the pancreas, leading to pancreatitis. This inflammation of the pancreas can be extremely painful and even life-threatening in severe cases. It is essential to be aware of the symptoms, such as abdominal pain, fever, and nausea, and seek medical help if you suspect gallstones or pancreatitis. By understanding this connection, we can take steps to prevent and manage these conditions effectively.
VIEW MORE